Priority Areas - Stewardship: 4C Antimicrobials
The term ‘4C antimicrobials’ refers collectively to the following four broad-spectrum antibiotics, or groups of antibiotics: co-amoxiclav, cephalosporins, fluoroquinolones and clindamycin.
The use of simple generic antibiotics and the avoidance of these broad-spectrum antibiotics preserve them from resistance and reduce the risk of C. difficile, MRSA and resistant UTIs. Compared with narrow-spectrum antibiotics, broad-spectrum antibiotics are more likely to significantly change the gut flora, potentially allowing other bacteria, such as C.difficile, to become established.
Concerns regarding use of fluoroquinolone and quinolone antibiotics have recently been noted. Very rarely, patients treated with fluoroquinolone or quinolone antibiotics have suffered long-lasting and disabling side effects, mainly involving muscles, tendons and bones, and the nervous system. In October 2018, the European Medicines Agency recommended restricting the use of fluoroquinolone and quinolone antibiotics. It stated that in patients at risk of aortic aneurysm and dissection, these antibiotics should only be used after careful assessment of the risks and benefits and after consideration of other therapeutic options. Patients should be advised of the importance of seeking immediate medical attention in case of sudden-onset severe abdominal, chest or back pain.
- Compared with narrow spectrum antibiotics, broad-spectrum antibiotics are more likely to significantly change the gut flora, potentially allowing other bacteria, such as C.difficile, to become established.
- The use of simple generic antibiotics and the avoidance of broad-spectrum antibiotics preserve these from resistance and reduce the risk of C.difficile, MRSA and resistant UTIs.
- These antimicrobials have a very useful role in specific clinical situations and should be reserved for use as per local guidelines.
Trend in 4C items per 1,000 patients
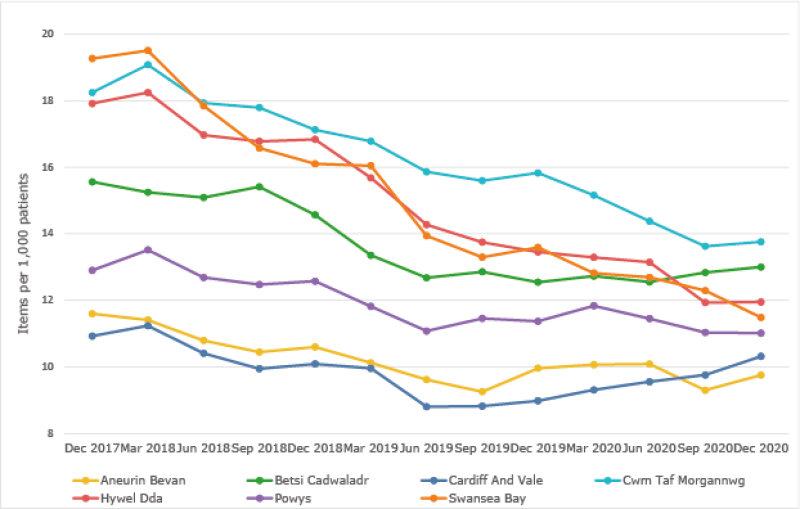
Total 4C antibacterial items per 1,000 patients – Quarter ending December 2020
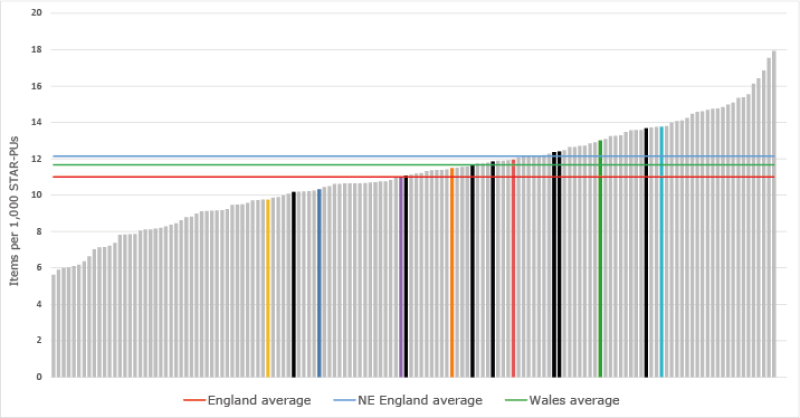
How can changes be made?
- Where an antimicrobial is indicated, follow local or national guidelines, prescribing antibiotics for the shortest effective course at the most appropriate dose.
- Consider the risk of antimicrobial resistance for individual patients and the population as a whole.
- Document and code the clinical diagnosis and reason for prescribing, or not prescribing, an antimicrobial.
- Consider a delayed/back up prescription.
- Provide patients with leaflets/resources so they are aware of how long they can expect their condition to last and how they can self-care. Resources are available in the TARGET Antibiotics toolkit.
- Carry out the AWMSG National Audit: Focus on Antibiotic Prescribing.

