Acute Low Back Pain Management
If the patient is still not returning to work, or unable to return to normal activities (if not employed) after 2-3weeks, the patient may seek further advice on their low back pain from healthcare professionals listed in 'Information resources for patients and carers'. At this point the patient should receive an assessment of their low back pain by an appropriately trained professional to rule out red flags and to discuss any psychosocial factors (yellow flags) that need to be addressed. Although the ‘flag’ system is not as popular as when it orginally was published, it is a good way of remembering about which factors to assess for.
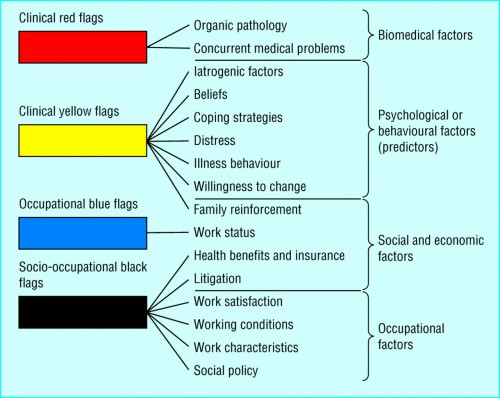
Figure 2: Flag system
Screening tools are useful in the assessment of psychosocial factors that may be affecting the patient’s recovery. They formalise the areas of questioning when probing for ‘Yellow flags’. They may be completed before the consultation in the waiting room so that no time is wasted and the responses may form a basis for discussion with the patient.
One useful tool to access psychosocial issues in the STarT back screening tool (there are many others from which to choose, but this is gaining in popularity). This assessment tool helps the correct identification of those LBP patients at risk of developing chronicity and aids the implementation of appropriate treatment (http://www.keele.ac.uk/sbst/.)
- Low risk - suggests patient will probably settle with appropriate advice and analgesia- return to primary care online if symptoms not settling
- Medium risk - suggest higher level of vigilance, plan review in primary care in 1-2 weeks, consider referring to information, advice, analgesia and/or therapies if not improving
- High risk - suggests significant risk of developing chronicity - consider early referral to secondary care chronic pain service / Community pain assessment and management service
The early assessment and treatment of patients at risk of developing chronic pain has been found to be effective at preventing long-term disability and chronicity.

